Q&A with Dr. James Hill, TCHMB's New Obstetrics Committee Co-Chair
In June of 2021, TCHMB Executive Committee was joined by two new Co-chairs of the Obstetrics Committee, Gloria Delgado and Dr. James Hill. We spoke to Dr. Hill to learn more about his experiences as TCHMB Co-chairs so far and his visions for the future of TCHMB.
In June of 2021, TCHMB Executive Committee was joined by two new Co-chairs of the Obstetrics Committee, Gloria Delgado and Dr. James Hill. We spoke to Dr. Hill to learn more about his experiences as TCHMB Co-chairs so far and his visions for the future of TCHMB.
Tell us a little bit about yourself.
I am currently the Division Chief for the Division of Maternal-Fetal Medicine at the Baylor College of Medicine in San Antonio. My interest in OB GYN started during the early years of medical school. Since completing my fellowship in Maternal-Fetal Medicine, I have worked in a number of rural and small community hospitals. During that time period, I recognized that many hospitals were deficit in personnel and material resources critical to providing the necessary care for some of the most complicated cases. I developed protocols and clinical guidelines for many of these hospitals. Years later, I was invited to join a workgroup of obstetricians, community physicians, maternal-fetal medicine physicians, neonatologists and epidemiologists to discuss the infrastructure for building a maternal and neonatal quality and safety regionalization system in Virginia. This is where my passion for improving maternal health took off.
How do you feel about joining the TCHMB executive committee?
I feel prepared. I have a special interest in quality improvement and I've been an active committee member on various quality improvement projects that have provided me with the experience needed and a better understanding for this position. I’m also excited to work with a number of experienced leaders and dedicated healthcare workers that are dedicated to improving the quality of care that we provide across the state of Texas and the opportunity to continue my efforts of reducing disparities, and maternal morbidity and mortality on a much broader level.
What do you hope to accomplish?
One of my main clinical and research interest is preeclampsia. And so I am excited that the TCHMB Executive approved the Obstetric committee’s most recent project proposal, titled Recognition and Response to Postpartum Preeclampsia in the Emergency Department.
This is a project that focuses on preeclampsia care in the emergency department. I hope to see that project move forward and implemented across the state of Texas.
What made you interested in the quality improvement aspect of healthcare?
The reduction of maternal mortality and morbidity has been and continues my career long passion. As an African American provider caring for pregnant women, I have a unique perspective regarding healthcare disparities. I have been very fortunate to have this opportunity, but many others who are minorities may not have. I am most alarmed at the dismal survival rates for African American mothers and their infants across the United States and Texas. Reading that women of color and black infants are dying at an alarming rate from preventable pregnancy-related complications is disturbing. I have not quite figured things out yet, but I want to help.
What appealed to you about the TCHMB executive committee that made you want to join?
The executive committee has many folks who are extremely experienced and through the collaboration with community stakeholders have put together many projects and quality initiatives that I believe identify the correct priorities. I’ve seen the work they have produced, and listened to their discussions, to where I feel confident that the right messages are being delivered with the right focus to advance health care quality and patient safety for all Texas mothers and babies through the appropriate collaboration.
Have you got to do anything interesting during your time so far as chair?
I have enjoyed working with a number of the committee members over the past few weeks. Namely, Dr. Davidson, the former Obstetric committee chair, who brings a tremendous amount of experience and guidance for my new position. The Texas AIM committee members have also been instrumental in putting together our postpartum project. I would also like to give a loud shout out to Nagla Elerian, who has been the strong leader of this organization and helps to keep the pieces from falling apart. Lastly, it has been great to have Gloria Delgado, as a co-chair. She has an unwavering commitment and is a well-respected and knowledgeable nurse that will help make this position a positive experience.
What is the proudest accomplishment of your career?
While my life has exposed me to many career opportunities and occupations of interest, there have only been a few professions I have every seriously considered. These are as follows: military service, medicine, teaching and the clergy.
I have always had a strong desire to have a career in the military. My desire for a military career initially stemmed from romantic notions of what such service entailed. These notions were replaced by a sincere need to feel as though I was doing my part in protecting that which I so fervently believe in, namely, our country and way of life. With that though in mind and my desire to serve in the armed forces, I decided that West Point was the best place to start my training. My outstanding 30-year career performance in the US Army has been a testament regarding my feelings about service to this country.
Things you are most excited about with your time on the TCHMB executive committee?
I’m most excited about having the support from the committee in working on the preeclampsia initiative in the emergency departments. This project is modeled after similar successful projects conducted in California, Florida and Illinois. I genuinely think this will allow us to improve care in not only the emergency departments, but also encourage collaboration with the OB units with a special emphasis on the care patients receive in the emergency departments.
Q&A with Gloria Delgado, TCHMB's New Obstetrics Committee Co-Chair
In June of 2021, TCHMB Executive Committee was joined by two new Co-chairs of the Obstetrics Committee, Gloria Delgado and Dr. James Hill. We spoke to both Gloria Delgado to learn more about her experiences as TCHMB Co-chair so far and her visions for the future of TCHMB.
In June of 2021, TCHMB Executive Committee was joined by two new Co-chairs of the Obstetrics Committee, Gloria Delgado and Dr. James Hill. We spoke to Gloria Delgado to learn more about her experiences as TCHMB Co-chair so far and her visions for the future of TCHMB.
Tell us a little bit about yourself.
I was born and raised in Mexico where I developed an early interest in STEM subjects. These interests brought me to college in the United States where I initially planned on studying engineering, however, my passions led me to nursing school. Since then, I have gained 25 years of experience as an obstetrics nurse at The Hospitals of Providence and now the University Medical Center of El Paso.
How do you feel about joining the TCHMB executive committee?
It is challenging but exciting. Working on a program like [the Recognition and Response to Postpartum Preeclampsia in the Emergency Department project] on a state level is something that is new to me. Working with physicians on a first name basis takes a little bit to get used to but everyone at TCHMB has been so kind and helped me greatly. I’m especially excited to join the committee because the work we are doing directly impacts the entire state of Texas.
What do you hope to accomplish?
During my time here, I wish to both learn and help patients deal with the issues I see personally. One problem I see at the hospitals I work at is hypertension in the obstetrics unit. I hope to make it so that people dealing with hypertension can get medication and treatment quickly.
What made you interested in the quality improvement aspect of healthcare?
Quality improvement is something that is considered rather new in the obstetrics department. Compared to other aspects of medicine where quality improvement initiatives were implemented for the past 20 years, in obstetrics we just started 3-4 years ago. We are extremely new to the system so I wanted to learn as much as I can about quality improvement so that we can implement it into obstetrics units across the state.
What appealed to you about the TCHMB executive committee that made you want to join?
Ever since I was in nursing school more than 20 years ago, I’ve always heard that El Paso was behind compared to other cities in Texas for healthcare. Since then, I’ve asked myself why El Paso is behind when the city is just as capable and competitive as any other city. When I heard about the initiatives for TCHMB and its goal to improve healthcare for the entire state of Texas, I was extremely interested.
Have you got to do anything interesting during your time so far as chair?
Meeting all the people involved in TCHMB has been such a rewarding experience for me. During my career, I’ve usually been exposed to a power dynamic between the physicians and nurses where we’re not seen as equals. My time at TCHMB has allowed me to talk amongst physicians without fear of being undermined or not taken seriously. These moments have made me realize how fortunate I am to be a part of this collaborative.
What is the proudest accomplishment of your career?
As the Administrator of Women’s Services at the hospital I work at, I was extremely proud to see that our hospital was awarded the “no findings” level designation for the second time. Our whole team worked remarkably to earn this designation, and to be in a position of leadership during all this was certainly a highlight of my career.
Things you are most excited about with your time on the TCHMB executive committee?
I’m most excited to learn from everyone. I want to learn more about quality improvement and how I can implement it into my own hospital. Since I’m now a part of TCHMB, I can now also help neighboring hospitals that are facing similar issues. This opportunity to help on a broader scale is what excites me most.
Collecting, Stratifying and Understanding Race, Ethnicity and Language (REaL) Data in Healthcare
Please join us on October 22 from 12-1 p.m. CDT for the first in our series of free webinars on collecting, stratifying, and understanding race, ethnicity, and language data in healthcare.
Please join us on October 22 from 12-1 p.m. CDT for the first in our series of free webinars on collecting, stratifying, and understanding race, ethnicity, and language data in healthcare. The goal of this first webinar is to provide a "farm to table" overview of REaL data collection and use. Future webinars will go into more depth into the different aspects of the process. Topics covered will include:
The “life cycle” of REaL data in Texas hospitals from collection to use in reporting and visualizing maternal and infant health outcomes by race, ethnicity, and language
Standards and processes for collecting accurate and complete REaL data
Who at your institution needs to be involved to improve the collection and use of REaL data for quality improvement in maternal and infant health
The Texas Collaborative for Healthy Mothers and Babies (TCHMB) is a multidisciplinary network made up of health professionals throughout the state. We are dedicated to the goal of reducing disparities in the health outcomes of mothers and babies in Texas.
---
Continuing Medical Education:
This activity has been planned and implemented in accordance with the accreditation requirements and policies of the Texas Medical Association (TMA) through the joint providership of The Texas Department of State Health Services, Continuing Education Service and The University of Texas Health Science Center at Tyler. The Texas Department of State Health Services, Continuing Education Service is accredited by TMA to provide continuing medical education for physicians.
The Texas Department of State Health Services, Continuing Education Service designates this live activity for a maximum of 1.00 AMA PRA Category 1 CreditsTM. Physicians should claim only the credit commensurate with the extent of their participation in the activity.
Continuing Nursing Education:
The Texas Department of State Health Services, Continuing Education Service is accredited as a provider of continuing nursing education by the American Nurses Credentialing Center’s Commission on Accreditation.
The Texas Department of State Health Services, Continuing Education Service has awarded 1.00 contact hours of Continuing Nursing Education.
Certified in Public Health
Up to 1.00 CPH Recertification Credits may be earned at this event.
Licensed Professional Counselors:
Up to 1.00 LPC hours may be earned at this event.
Licensed Psychologists:
The Texas Department of State Health Services, Continuing Education Service is approved as a provider of professional development hours for licensed psychologists, per the Texas Administrative Code Rule §463.35 (f)(1). The Texas Department of State Health Services, Continuing Education Service has awarded 1.00 professional development hours.
Social Workers:
The Texas Department of State Health Services, Continuing Education Service, the continuing education provider, ensures that the education provided is directly related to the practice of social work; and that the individuals presenting the information have the necessary experience and knowledge in the topics presented. The Texas Department of State Health Services, Continuing Education Service has awarded 1.00 hours of credit.
Certificate of Attendance:
The Texas Department of State Health Services, Continuing Education Service has designated 1.00 hours for attendance.
Q&A with Dr. Patrick Ramsey, TCHMB Chief Medical Officer
Meet Dr. Patrick Ramsey, the Chief Medical Officer of the Texas Collaborative for Healthy Mothers and Babies.
In September of last year, Dr. Patrick Ramsey stepped down from his position as Vice Chair/Chair Elect of the TCHMB Executive Committee in order to serve in a staff role as TCHMB’s first ever Chief Medical Officer. It was a milestone for TCHMB, which launched in 2013 with strong leadership at the Executive Committee level but no one in the CMO role that has been so instrumental to the success of many of the nation’s more established perinatal quality collaboratives.
“Pat was an obvious choice,” says Dr. David Lakey, who helped launch TCHMB when he was Texas state health commissioner and now serves as a member of the Executive Committee. “He has a strong background in both research and quality improvement. He’s been with TCHMB for years, and he was already in a leadership role. And he has the vision and commitment to help take the Collaborative to the next level.”
In addition to his role as CMO, Ramsey is a Professor and Division Chief for Maternal-Fetal Medicine at UT Health San Antonio. He is an active member of the American College of Obstetricians and Gynecologists, the Society of Maternal-Fetal Medicine, and the Infectious Disease Society for Obstetrics and Gynecology, among other organizations. And he is an active researcher and educator, with numerous awards and accolades and more than 100 peer-reviewed papers in major journals. His research interests are clinical trials, prevention of preterm birth, reduction of maternal morbidity and mortality, and management of medical complications of pregnancy.
We spoke to Ramsey about his background, his path to the TCHMB, and his vision for its future.
From where do you hail and how did you end up in Texas?
I’m from Wisconsin originally. I came here with my wife in 2009. She was a military Ob-Gyn and was assigned to a base in San Antonio. I went to a high-risk pregnancy practice, and then moved over to UT Health San Antonio.
What brought you to TCHMB?
I received an email through the Perinatal Advisory Council that there was an opening. At the time, I didn’t know a lot about TCHMB other than that it was the state perinatal quality collaborative. I knew that the California PQC had done a lot of amazing work, and thought it would be exciting to be involved at the ground level with something that could potentially become very important.
When did you get the QI bug?
I’ve always been interested, as a physician, in evidence-based practice, and in translating research into clinical practice. A lot of my past research has focused on how to prevent women from having a pre-term or recurrent pre-term delivery, and in how to optimize outcomes in women who do deliver preterm. That very naturally led to getting involved with quality improvement work at UT Health San Antonio. That in turn is what led me to the Data Committee on TCHMB.
Your position, Chief Medical Officer, is a new one for the Collaborative. Can you talk about that?
Many of us in the upper leadership of TCHMB came to the realization that the way we were doing things was not sustainable. If we wanted to have the same kind of impact that some of the other PQCs around the country have had, we needed to have a medical leader who could dedicate him or herself more fully to expanding the footprint and visibility of these initiatives. We couldn’t just depend on voluntary service, though that still plays a big role in the operations of the Collaborative. So we created the chief medical officer position.
That was a critical step to making sure we had a bigger impact in the state, and over time more visibility nationally. The even more critical change has been the integration with the RAC-PCR Alliance, which is the implementation arm on the ground. That merger really kicks us up in terms of the level of impact we can have.
Why is the merger so important?
For so many reasons. The RACs and PCRs are the conduit to the hospitals. They are the hospitals. Merging with them is what is going to allow us to implement QI initiatives at a truly state-wide level, which will allow us over time to have a measurable impact on outcomes for mothers and babies. At the same time, TCHMB as an entity has capacities they don’t, in terms of providing QI training, ongoing coordination of initiatives, and coordination of a diverse array of stakeholders from across the state. We have the same goal, but we have different strengths to bring to the table. We need to work together, and now we are.
Q&A with Dr. Catherine Eppes, TCHMB Chair
Dr. Catherine Eppes, the new chair of the Texas Collaborative for Healthy Mothers and Babies (TCHMB), has set herself two straightforward but challenging goals for the next two years.
Dr. Catherine Eppes, the new chair of the Texas Collaborative for Healthy Mothers and Babies (TCHMB), has set herself two straightforward but challenging goals for the next two years. She would like to 1) help drive the establishment of a robust data infrastructure for hospitals to report and receive key quality improvement metrics, and 2) further strengthen the alliance between TCHMB and the Regional Advisory Council (RAC) Perinatal Care Region (PCR) Alliance.
“If we accomplish those two goals I will feel as though I have been successful,” says Eppes, who is a maternal fetal medicine physician at Baylor College of Medicine and the Chief of Obstetrics for Ben Taub Hospital in Houston.
Eppes, who was selected as chair after serving for three years as co-chair of the Obstetrics Committee, received her MD from The University of Texas Health Science Center, San Antonio and completed residency at Johns Hopkins. Her fellowship, and masters of public health, were received from Northwestern University. Her primary areas of focus are quality and safety and infectious diseases in pregnancy. She is currently the ACOG District XI (Texas) patient quality and safety chair, a member of the Texas fetal and infant review of HIV and Syphilis, and Faculty Medical Director of the TexasAIM initiative. She holds several grants with the CDC for influenza and HIV in pregnancy.
From where do you hail?
I was born in Maryland. My family moved to Texas when I was in junior high, and I did my undergraduate work at UT Austin. I moved away for medical school, residency and fellowship, and then came back here after my fellowship. I went directly to Ben Taub Hospital in Houston, which is the Harris County safety net hospital, and I’ve been at Ben Taub since.
Did you always know you wanted to be an OB-GYN?
I went to medical school thinking I wanted to be a neurosurgeon, but knew I wanted to be an OB-GYN by the end of medical school, and went to Northwestern University in Chicago for a fellowship in maternal and fetal medicine and a Masters in Public Health as well.
So it’s not an accident that you ended up with TCHMB, at the intersection of perinatal and public health?
I had some really amazing mentors at Northwestern, including Pat Garcia and Ann Borders (who would later be one of the keynote speakers at the 2019 TCHMB Summit). They were working not just on caring for women but on improving the systems that cared for (or in many cases didn’t care for) women. It was largely from watching those two women that I learned what kind of doctor I wanted to be.
How did you end up back in Texas?
I won the job lotto. I wanted to be back in Texas. Baylor College of Medicine is a major medical institution, operating at the highest levels of both research and clinical care. And Ben Taub, where I work, is the safety net hospital for Harris County. We’re the hospital that cares for patients who are medically underserved, the majority of whom are not insured and many of whom are undocumented. It’s an amazing place.
How did you make your way to TCHMB?
After the 2016 election, I felt very strongly that I wanted to be more involved in improving maternal health in our state. Christina Davidson, who is a good friend, had been involved with TCHMB for a number of years at that point, and she encouraged me to apply. I joined in January of 2017 as part of the Data Committee. I subsequently became one of the co-chairs of the Obstetrics Committee.
Where do you think TCHMB is, in terms of its development as a PQC?
We are still young, but I think we are more like a teenager now. Our committees are beginning to work together on projects. We have been through a few cycles of leadership. We have integrated with the RACs and PCRs. We have hired a chief medical officer. We have embarked on a QI project, the Newborn Admission Temperature (NAT) project, that is going to be our first that is truly statewide.
In combination with the work that DSHS has done with TexasAIM, the state has come a long way in only a few years, and other states are watching us now.
What’s next?
A lot, but the biggest thing we need to build, in my opinion, is a good data infrastructure. With the RAC-PCR integration, and the levels of care designation requirements that hospitals engage in QI projects, it is realistic that we can implement projects that involve all 224 of the birthing hospitals in Texas. We are going to get close to that with the NAT project alone. But without a good data infrastructure, and the reporting that it would allow, we will be limited in the impact we can have. That’s the big goal for the next two years, to get to a point where we have a common data infrastructure, where hospitals are submitting to one place, not multiple different places, and we and they can begin to use that data to drive improvement.
What are the big challenges in setting up such an infrastructure?
The technical challenges are significant but surmountable. What system are we going to use? What metrics will we collect? How will our system integrate with electronic health records? Etc.
Perhaps the greatest challenge, however, is persuading the hospitals to share. They have legitimate concerns about privacy, about their outcomes being visible to others, and about it potentially being punitive. We need to create a culture of trust where data is not used punitively.
What do you mean by punitive here?
Neither TCHMB nor the state is interested in using outcomes data to punish hospitals or systems, or to draw invidious comparisons. That would be punitive. Our goal is to provide data to empower hospitals to improve outcomes for mothers and babies, which they all want to do. Everybody really cares so much about improving their own outcomes, and they don’t need to be shamed to be motivated to improve. But knowing where they are, vis a vis other hospitals, can be incredibly helpful. You may be an outlier without knowing it.
Anything else?
I am really excited about the equity work that our Community Health Committee is doing, where the goal is to add that lens to every project we do going forward. I think it will be a hard and emotional journey for a lot of folks, but I think it’s the right time and the right group of motivated people, so I’m excited to see where that goes.
How do you feel about being selected as chair of TCHMB?
Honored.
Webinar: Introduction to TCHMB’s Newborn Admission Temperature Initiative
TCHMB invites you to participate in an introductory webinar for the NAT initiative on March 24 from 3-4pm.
TCHMB invites you to participate in an introductory webinar for the NAT initiative on March 24 from 3-4pm. This webinar will be the official launch of the project where we will be discussing more details about the initiative including the importance of tracking newborn admission temperature, the data measures, and techniques and strategies for data collection for the project. Please invite your NAT team members to participate in the webinar to learn more and prepare for the project.
When: Mar 24, 2021 03:00 PM Central Time (US and Canada)
Topic: Introduction to TCHMB’s Newborn Admission Temperature Initiative
Register Now for this webinar.
After registering, you will receive a confirmation email containing information about joining the webinar.
If you have any questions, please reach out to Dr. Meliha Salahuddin at nat@utsystem.edu.
Texas Collaborative for Healthy Mothers and Babies Welcomes New Leadership
The Texas Collaborative for Healthy Mothers and Babies (TCHMB) has named Dr. Catherine Eppes as Chair of its Executive Committee and Dr. Rashmin Savani as Vice Chair/Chair-Elect.
Austin, TEXAS - The Texas Collaborative for Healthy Mothers and Babies (TCHMB), Texas’s state perinatal quality collaborative, has named Dr. Catherine Eppes as Chair of its Executive Committee and Dr. Rashmin Savani as Vice Chair/Chair-Elect.
Stepping down as chair after a 2-year term is Dr. Michael Speer, Professor of Pediatrics and Neonatology at Baylor College of Medicine and Medical Director of the Neonatal Nurse Practitioner Program at Texas Children’s Hospital. Dr. George Saade, Chief of Obstetrics and Maternal-Fetal Medicine at the University of Texas Medical Branch, will step down from the Executive Committee after serving for over 4 years in the roles of Chair and Past Chair.
“Dr Eppes and Dr. Savani are extraordinary physicians and long-time champions of maternal and infant health in Texas,” says Speer, who will continue to serve on the executive committee as Past Chair for the next two years. “I couldn’t be more confident in the future of TCHMB.”
Catherine Eppes, MD, MPH, is a Maternal-Fetal Medicine physician at Baylor College of Medicine and the Chief of Obstetrics for Ben Taub Hospital. She received her MD from The University of Texas Health Science Center, San Antonio and completed her obstetrics residency at Johns Hopkins. Her fellowship, and Masters of Public Health, were received from Northwestern University. She is currently the ACOG District XI (Texas) patient quality and safety chair, and TexasAIM Medical Director. She holds several grants, including the maternal opioid misuse grant which is a collaborative grant between Texas Health and Human Services and Harris Health to improve the outcomes of women with substance use disorder. Prior to her selection as Chair, she served on the TCHMB Executive Committee as co-chair of the obstetrics committee.
“Texas has a lot of challenges when it comes to the health of its mothers and babies,” says Eppes. “We also have an extraordinary community of people dedicated to making things better. Under the leadership of Dr. Speer and his predecessor, Dr. George Saade, the Collaborative has been an important part of that larger community, and I look forward to carrying the mission forward.”
Rashmin Savani, MD, is Division Director of Neonatal-Perinatal Medicine and Associate Director of Pulmonary & Vascular Biology in the Department of Pediatrics at The University of Texas Southwestern Medical Center. He obtained his medical degree from the University of Sheffield and was a pediatric resident at Duke University Medical Center and a fellow in Neonatology and in Pulmonary Biology (1989-1991) at Cincinnati Children’s Medical Center. His research focus has been on lung injury and development, including inflammation and angiogenesis. Prior to his selection as Vice Chair/Chair-Elect, he served on the TCHMB Executive Committee as co-chair of the neonatology committee.
“This is a wonderful opportunity to work collaboratively with leaders across Texas to improve the health of moms and babies in Texas,” says Savani. “It’s a privilege to be selected as vice chair.”
Former Vice Chair Dr. Patrick Ramsey, Professor of Obstetrics and Gynecology at the University of Texas Health Science Center at San Antonio, now serves in a staff role as TCHMB’s Chief Medical Officer.
The Texas Collaborative for Healthy Mothers and Babies is a multidisciplinary network made up of health professionals throughout the state. Its mission is to advance health care quality and patient safety for all Texas mothers and babies, through the collaboration of health and community stakeholders in the development of joint quality improvement (QI) initiatives, the advancement of data-driven best practices, and the promotion of education and training.
MMMRC and DSHS Joint Biennial Report
The report contains DSHS and MMMRC findings and MMMRC recommendations to help reduce the incidence of pregnancy-related deaths and maternal morbidity in Texas.
The Texas Maternal Mortality and Morbidity Review Committee (MMMRC) and Department of State Health Services (DSHS) have jointly released their 2020 Biennial Report. The report contains DSHS and MMMRC findings and MMMRC recommendations to help reduce the incidence of pregnancy-related deaths and maternal morbidity in Texas.
Summary of Recommendations
Increase access to comprehensive health services during pregnancy, the year after pregnancy, and throughout the preconception and interpregnancy periods to facilitate continuity of care, enable effective care transitions, promote safe birth spacing, and improve the lifelong health of women.
Engage Black communities and apply health equity principles in the development of maternal and women’s health programs.
Improve access to integrated behavioral health care from preconception through one-year postpartum for women with mental and substance use disorders.
Improve statewide infrastructure and programs to address violence and intimate partner violence at the state and community levels.
Implement statewide maternal health and safety initiatives to reduce preventable maternal mortality and morbidity.
Foster supportive community environments and leverage programs and services that help women of childbearing age achieve their full health potential.
Support coordination between emergency and maternal health services, and implement evidence-based, standardized protocols to identify and manage obstetric and postpartum emergencies.
Improve postpartum care management and discharge education for patients and families.
Continue and strengthen activities to increase public awareness and prevention.
Support strategies to continuously improve maternal mortality investigation and case review processes.
The full report is available on the DSHS website.
Increasing Access to Healthcare Coverage for Uninsured, Postpartum Women in Texas
This first report from TCHMB’s PATH (Postpartum Access to Healthcare) project provides information on healthcare coverage during the postpartum period for underserved women, and provides recommendations for improving access to healthcare coverage, specifically through the Texas women’s health programs.
This report provides information on access to healthcare coverage during the postpartum period for underserved women, and provides recommendations for improving access to care, specifically through the Texas women’s health programs.
This report is a product of the Postpartum Access to Healthcare (PATH) Project, a study of the system and experience of care during the postpartum period for underserved women in Central Texas. PATH is a project of the Texas Collaborative for Healthy Mothers and Babies (TCHMB), the state perinatal quality collaborative, and is funded by the St. David’s Foundation.
Data sources for the PATH project and this report include interviews with 32 pregnant/postpartum women and with 20 providers and clinic staff who serve this population. Each woman was interviewed up to three times (late prenatal, 1-2 weeks postpartum, and 4-6 weeks postpartum). Qualitative interview data were supplemented with available quantitative data on Texas’ women’s health programs sourced from publicly-available Texas state agency documents. Participant recruitment was conducted in partnership with two large Federally Qualified Health Center (FQHC) systems in central Texas.
This study identified three key areas for action to increase access to public healthcare coverage for underserved women:
Close the information gaps among women, providers, and advocates regarding the Texas Family Planning Program and Healthy Texas Women and encourage provider participation.
Improve processes to facilitate women’s transition between Medicaid for Pregnant Women and Healthy Texas Women.
Bolster the Texas Family Planning Program to expand its reach and scale its impact.
Letter from the Chair and Executive Sponsor
Like so many organizations, the Texas Collaborative for Healthy Mothers and Babies has been engaged in a conversation about how to stay true to our commitments while adapting to the realities of a health care system that has had to shift priorities in ways we couldn’t have anticipated even two months ago.
Dear Friends and Colleagues,
Our thoughts are with you and your families as you do your best to weather the COVID-19 crisis.
Like so many organizations, the Texas Collaborative for Healthy Mothers and Babies has been engaged in a conversation about how to stay true to our commitments while adapting to the realities of a health care system that has had to shift priorities in ways we couldn’t have anticipated even two months ago.
In light of this new reality, we will continue with our current quality improvement programs, but will shift deadlines, expectations, and metrics as needed. The leadership and committees will continue to meet, but will do so remotely and in some cases less often. We will continue to communicate about our initiatives through our newsletter and on social media, but will do so less frequently than before. We will also post perinatal-specific resources on dealing with COVID-19 on our website.
Paid staff at UT System will continue to dedicate their time to TCHMB as before, but much of the clinical leadership on the committees and in the hospitals and clinics may not be able to dedicate as much time as they were prior. And we will all continue to adapt as the situation changes.
Stay safe, and please reach out with questions and suggestions.
Sincerely,
Michael E. Speer, MD
Chair, Texas Collaborative for Healthy Mothers and Babies
David Lakey, MD
Vice Chancellor for Health Affairs and Chief Medical Officer, The University of Texas System
TCHMB Wins 2nd Place in National Improvement Video Challenge
The TCHMB-produced video, “MEWS: A Simple Alogorithm for Reducing Maternal Mortality and Morbidity, has been awarded second place in the Council on Patient Safety in Women’s Health Care’s National Improvement Video Challenge.
The TCHMB-produced video, “MEWS: A Simple Alogorithm for Reducing Maternal Mortality and Morbidity, has been awarded second place in the Council on Patient Safety in Women’s Health Care’s National Improvement Video Challenge.
Diabetes Screening and Treatment Available for Healthy Texas Women Clients
To learn more about which medications are covered, healthcare providers can access the HTW specific formulary at txvendordrug.com/resources/downloads.
Healthy Texas Women is a program dedicated to offering women’s health and family planning at no cost to eligible women in Texas. Since July 1, 2016, the HTW program has provided coverage for screening and treatment of hypertension, diabetes and high cholesterol.
In the most recent Maternal Mortality and Morbidity Task Force and Department of State Health Services Joint Biennial Report, chronic health diseases such as pre-pregnancy obesity, diabetes and hypertension were all associated with an increased risk for maternal death. The Centers for Disease Control and Prevention reports that almost 25 percent of people with diabetes and 20 percent of people with hypertension are undiagnosed.
By increasing access to vital health services and treating underlying medical conditions, women’s health and pregnancy related outcomes can improve in Texas.
Several commonly prescribed medications used to treat these conditions are available on the current HTW drug formulary. Clients approved for HTW can get these medications at any Medicaid participating pharmacy with their program identification card.
To learn more about which medications are covered, healthcare providers can access the HTW specific formulary at txvendordrug.com/resources/downloads. Participating HTW providers can access information regarding policies, billing guidelines and toolkits at healthytexaswomen.org/provider-resources.
An Alliance Is Born: Jeanne Mahoney on the Birth and Growth of the Alliance for Innovation in Maternal Health Care (AIM)
We speak to Jeanne Mahoney, Director of the National AIM initiative, about the origins of AIM, the reasons for the rise in maternal mortality, and the development and dissemination of AIM’s bundles.
For most of the past century, the trend in maternal mortality in the US was a good one. Fewer women were dying in connection with their pregnancies. The trend was so good in fact, that many states and cities retired their maternal mortality review committees. They didn’t seem necessary anymore.
Then something changed. Beginning in the mid-2000s, the numbers started going in the wrong direction. More mothers were dying.
Over the past decade, a new infrastructure has emerged to address that critical and tragic trend. At the center of it is the Alliance for Innovation in Maternal Health Care (AIM), which Jeanne Mahoney directs through her work for the American College of Obstetricians and Gynecologists (ACOG). 28 states (including Texas) are now implementing AIM safety bundles, with the remaining 22 states either intending to get involved or exploring involvement.
We spoke to Mahoney, who was an invited speaker and panelist at the 2019 TCHMB Summit, about the origins of AIM, the reasons for the rise in maternal mortality, and the development and dissemination of AIM’s bundles.
Mahoney came to ACOG in 2002 from the Massachusetts Department of Public Health, where she was involved in coordinating risk reduction programs for women of reproductive age.
---
TCHMB: What’s the story behind AIM? I was looking at the maps you showed at the conference, of the recent and rapid spread of AIM states, and it’s all very recent, isn’t it?
Jeanne Mahoney: Yes and no. In a way it starts in 1992, when a group of people interested in maternal mortality began getting together at the annual ACOG meeting. It was OB/GYNs, public health people, anesthesiologists, all sorts of people who were engaged with women’s health. At the beginning the group wasn’t meeting with a sense of alarm. The numbers had been going down for decades, and the assumption was that they would continue to do so. Then around 2008, we started seeing these numbers rising, and that changed the tenor of the discussion.
Elliott Main had been tracking the numbers in California and seeing the same kind of rise. It became very clear that it was a real problem, not just a statistical fluctuation.
We pulled together a group in 2012 to do a real deep dive into the data and to begin to formulate a national response. What we saw was that there wasn’t just one cause of the rise in maternal mortality. There were many overlapping causes, as well as a great deal that we didn’t yet understand. What we saw clearly, though, were two major cause that were remediable, maternal hemorrhage and hypertension. These were issues about care that we could do something about there and then.
At the national ACOG meeting that year we had a big meeting of about 150-180 people. We came to a consensus that we would begin to develop and deploy maternal safety bundles. We called the group the National Partnership for Maternal Safety. It was not really a card-carrying organization, but it helped formalize the structure. Out of that came The Alliance for Innovation on Maternal Health (AIM), which is staffed by us here at ACOG but is a true alliance. There are 30 different partners across multiple sectors that work with us on every aspect of AIM.
Why did the maternal mortality numbers start going up after so many years of progress? I realize it’s complex, and there are really long answers to that question, but what’s the short version?
For the two issues that we started out with, maternal hemorrhage and hypertension, I can give you some relatively straightforward answers that explain a least a substantial part of the cause.
With maternal hemorrhage we call it “too much too soon too little too late.” We are not waiting for women to have their babies. As a culture we started doing more inductions, more c-sections. We kept pushing the envelope. We have been inducing labor in too many women who don’t have medical reasons for induction, and if the babies fail to arrive on schedule, during an induction, we give the mother more and more oxytocin, and that can be dangerous.
Oxytocin causes the uterus to contract, and the uterus is a muscle like any other muscle. If you force it to contract over and over, it gets tired. After birth it is supposed to contract hard, but too much oxytocin can increase the risk of it failing to contract while the uterine blood vessels continue to pump blood—up to 1/8th of a woman’s total blood volume per minute. The risk increases the longer it takes us to recognize the bleeding.
There is a different hypertension story. Blood pressure has been going up overall in pregnant and postpartum women. We’re not entirely sure why, but that increase has intersected with a slowness, on the part of providers, to implement best practices in how to manage the blood pressure of pregnant and postpartum women.
The walls of the blood vessels of women who are pregnant and early postpartum are very thin, and so the vessels can leak at lower blood pressures than in other people. For a long time that wasn’t the training we were getting. We were taught that the danger zone for pregnant and postpartum women was the same as in other people. We know now that the danger threshold is lower than for the general public. The systolic number, the top number, should never go above 160. Normally we don’t start to treat blood pressures until that systolic number is over 180. By that point, a pregnant or early postpartum woman is much more susceptible to having a stroke and dying.
We have to retrain our providers on every level to be able to understand the hemodynamics of pregnancy and postpartum, so we aren’t sending women home from the hospital early, and we are responsive when they are exhibiting warning signs.
Another big part of the story is women dying from drugs and particularly opioids. Those are mostly killing women post-partum. In Texas right now, for instance, that is accounting for about 50 percent of maternal mortality. One of the ways this is happening is that during pregnancy, many women get some kind of medication assisted treatment for opioids, but then Medicaid runs out 42 days postpartum. Soon after, they go straight to street drugs to treat their disease of addiction, and they overdose and die far more frequently than women using opioids who have not been pregnant.
So how did you get from that big meeting in 2012 to the actual development and deployment of safety bundles? To the official launch of AIM?
We decided our bundles were going to be evidence-based best practices, and that we would pull together a team of experts to develop them. It was multi-disciplinary work-groups of 10-15 people who had to come to consensus. The groups included nurses, doctors, the head of the American Blood Bank Association, someone from the national obstetric anesthesiologists association, and others.
It was hard to come to consensus, having that many different organizational folks sitting around the table. Our hemorrhage bundle, for instance, took us almost two years, because we needed to learn how to work together. At the same time, that process was immensely valuable, both on its own terms and because when we finally did achieve consensus, we already had those organizations on board, affirming this work.
The key with the bundles is that they are very specific in certain ways, and very open in others, so that the hospitals have a lot of flexibility in how they implement them. These are the practices that you need to do, and now you figure out how to do it. If we talk about a medication, for instance, we don’t put dosages in, or instruct providers how to give them. That makes it a lot easier on the implementation end, and so our bundles endure. The hemorrhage bundle, which we developed in 2013-2014, hasn’t changed at all. We review it every 18 months or so, to see if it still applies, and although we have added some references, the itself bundle remains the same.
How did you get the bundles out into the world? It is one thing to have a good set of tools. It’s another thing to get people to use them, and to find the resources to support that.
We began working on the bundles in 2013. In 2014 we applied for and received a grant from the Maternal and Child Health Bureau at HRSA for what we were now calling the Alliance for Innovation on Maternal Health, or AIM. We came out with the hemorrhage and hypertension bundles around then, and then we kept going. We now have 10 bundles, including bundles on venous thromboembolism prevention, postpartum care, reduction of racial disparities, and opioid use disorder.
In terms of getting buy-in more broadly, it helped that from the outset we had support from the broad coalition of organizations involved in the development of the bundles. They were partners in the grant application and gave us credibility as well as avenues for dissemination and outreach. We also worked out a really unique deal with the major disciplinary journals for the simultaneous publication of the commentaries that add implementation support to each bundle. These commentaries flesh out the bundles with definitions, references, discussion of issues that need more discussion, and so on. Whenever we release a bundle the commentary is published in three to five separate peer reviewed journals simultaneously.
Even with all that support, though, at first we were hard pressed to find states to participate. No one understood what we were doing, and we had to sell them on it. Over time, as we’ve established ourselves, and demonstrated the efficacy of the bundles, getting buy-in has become easier.
What is the efficacy?
We are seeing in the hospital outcome data that the states that are doing any bundle at all have reduced their severe maternal morbidity rates 8-25% across the board. A lot of that improvement, we believe, is the result of just pulling the teams together and working on an issue together. It is changing the way people are thinking. They are working together, and that produces good outcomes.
Do the bundles make the work of providers harder? Is it more work?
Yes and no. The bundles themselves are best practices we should be doing anyway. They’re substituting more effective practices for less effective practices. The data part is a little trickier, because in many cases it is adding several process and structure measures that need to be entered into a data system. Doing rapid cycle data driven quality improvement provides the basis for action and is highly valued.
You mentioned the racial disparities bundle. That feels like a very different challenge to tackle than the other bundles. It’s one thing to say that you should always have a hemorrhage cart nearby in situations x and y. It’s very different to tell providers to be less racially disparate, when we don’t even know most of the causes of racial disparities.
It is very tricky, and also very important. We see these incredible disparities in morbidity and mortality. But also variation in the degree of disparity, which suggests that there is a lot of room for improvement. New York City, for instance, has a twelve-fold difference between black and women dying. Illinois has a six-fold difference. Across the country we are seeing a 3 to 4-fold higher rate of black maternal mortality.
This is not just about black women coming in with higher risk factors. One thing we are finding is that there are communication issues. We are not listening to some women as well as we are to others. So somebody says, “I am having pain,” and instead of exploring the possible causes of that pain, the response is, “You’ve just had a baby, of course you have pain.” That happens more to black women than white women. We need to find ways not just to close the gap but to improve communication with all women.
Right now we have a grant from the Robert Wood Johnson Foundation to try to quantify those voices of women, to develop measures that we can track and give back to providers to let them know how they’re doing and how they can improve.
That sounds fascinating, but hard. How would you do that? How do you quantify that kind of subtle communication?
It’s complicated. The grant with RWJ involves studying interactions and identifying key words and phrases that can signal, for instance, that communication is failing. And not just words, nonverbal communication as well. The goal will be to train medical providers to be alert for those key words and gestures that signal that they need to listen more closely. And not just the physicians, the other providers as well, so that there are multiple people listening to and looking out for women.
It is not going to be easy work, but we have hospitals who want to be part of the pilots, which is an indication of the interest in addressing the issue.
One thing I noticed at our conference this year was how many nurses were there. That surprised me, but it probably shouldn’t have. Is that true nationally?
Yes. In every meeting we have for AIM, there are more nurses than docs. Some of that is a result of who the hospitals are choosing as their representatives. They’re more likely to send nurses. But it’s also because nurses really like this work, because it empowers them to provide the best care for their patients. They’re not having to negotiate conflicting instructions from different doctors, and in many cases, it provides them the means to intercede if the care is not being provided according to the bundle.
What’s on the horizon for AIM?
We’re working with more and more states, like Texas, on implementing bundles. We have projects that are focusing on improving care, and customizing bundles, for rural settings. We are rural-izing them, as one of our partners in North Dakota said. We are doing work internationally. Did a project in Malawi, for instance, in which were able to reduce maternal mortality due to hemorrhage in three hospitals by 83%.
We’ll keep working to improve the health of mothers.
Three Things: Dr. Ann Borders on What Makes or Breaks a Perinatal Quality Collaborative
We spoke to Dr. Ann Borders, Executive Director of the Illinois Perinatal Quality Collaborative (ILPQC), about how state perinatal quality collaboratives can make a real difference in the lives of mothers and babies.
When Dr. Ann Borders was tapped to help launch the Illinois Perinatal Quality Collaborative (ILPQC), her first move was to ask for help. Other states had successfully launched and developed PQCs. Illinois’ best bet for achieving its own success, she knew, was to learn from them.
“We asked them, ‘If you were starting a new PQC what would you do?’” said Borders, Executive Director and Obstetric Lead for the ILPQC. “Then we went home and tried to imitate that.”
They succeeded. In the five or so years since, Illinois has emerged as one of those states worth imitating in its own right, with over 100 birthing hospitals participating in its initiatives and an impressive record of improving outcomes for mothers and babies. Borders herself has emerged as a national expert on creating, growing, and sustaining a PQC, and now serves on the National Network of Perinatal Quality Collaboratives Executive Committee.
We spoke to Borders after her keynote speech at the 2019 Texas Collaborative for Healthy Mothers & Babies Summit.
—-
Dr. Ann Borders at the 2019 Texas Collaborative for Healthy Mothers and Babies Annual Summit
TCHMB News: When you first were launching the Illinois Perinatal Quality Collaborative (ILPQC), what did you do to maximize the chances of success?
Dr. Ann Borders: We started with that premise that we needed to learn from successful collaboratives, in states like Ohio, California, Florida, and North Carolina. We very specifically sought their input.
I remember we got a team together from Illinois to attend the annual meeting of the Florida PQC. We flew down there, and set up meetings with the Florida leadership, which was led by Bill Sappenfield, as well as with Jay Iams from Ohio, Elliott Main and Jeff Gould from California, and Marty McCaffery from North Carolina.
We asked them: How did you put a structure together? How did you create a data system? How do you interact with your teams? What are pitfalls to avoid? What are the key steps to be successful with stakeholders? We went home and tried to imitate their recommendations.
Illinois is now seen as one of those PQCs that knows how to make it work. You’re brought in (to Texas, for example) to help newer PQC launch and grow. From your perspective, what’s the secret?
From our experience, the collaboratives that make it work provide value to the hospital teams. I’d break that down into three strategies that are key to this work:
Provide opportunities for collaborative learning, getting teams together to share and learn from each other, whether that’s in person or through calls and webinars.
Have a rapid response data system that hospitals can really utilize to compare data across time and across participating hospitals to effectively drive QI.
Provide quality improvement support, primarily with QI coaching calls and follow up. Teams may also need site visits with key player meeting when appropriate or small group discussion calls to link up higher performing hospitals with hospital teams still struggling with a particular QI topic. The goal is to help every hospital succeed.
What about the ones that aren’t as effective? What are they doing wrong, or failing to do?
Every state is different in terms of the stakeholders, the funding, and the available infrastructure, so it is never one size fits all. We do think, however, that there are some strategies that may help teams achieve success more efficiently and hopefully more effectively. We also believe that every PQC has something to learn from every other PQC, no matter how long they have been at this work. Collaborative learning across PQCs is just as important as collaborative learning across hospitals in order to achieve success.
In our experience, we have found it important to use a quality improvement model, have access to rapid response data, and have an infrastructure that provides regular communication with hospital teams and opportunities for collaborative learning. Collaboratives seem to be more successful when they focus on quality improvement strategies to help their hospital teams be successful. Also successful collaborative teams focus on one or maybe two initiatives at a time. They don’t try to take on too much. They have clear aims and only collect data that helps hospitals drive change and show progress towards improvement. They stay focused on helping teams implement clear, measurable system changes and culture changes at primarily the hospital level (some collaboratives have successfully added outpatient settings, though it can be more of a challenge).
I think some collaboratives may fall into the trap of taking on too much when getting started, and this can be a hard way to start. It can be hard not to do this when stakeholders are pushing collaboratives to be responsive across a number of areas, but teams can feel overwhelmed when asked to do too much and it is hard to show effective improvement. This can be frustrating for everyone. It should be clear what the strategies are for improvement and what the aims are for demonstrating success. In our experience, staying focused is important for PQCs to be successful and for helping hospitals succeed.
As the PQC movement has developed, there have been some collaboratives that started with more of a public health model: needs assessment, project implementation with education and resources, and then evaluation with vital record data or other population health data. That is a model that can work well in many public health settings, but it does not seem to support rapid-cycle quality improvement through implementation of systems and culture change in the same way as the strategies that we now see most PQCs embracing.
From our experience in Illinois, and in collaborating with other state PQCs, it is hard for hospitals to wait six months or a year for data on efficacy. It is hard to be able to successfully use that data to drive quality improvement. Teams that have access to rapid response data with easy to use reports can most easily use that data for quality improvement. Also many hospital teams need QI support, because hospital teams don’t all have the same experience and infrastructure to support quality improvement. Also we have found that hospital teams benefit if they are able to learn in real time from other hospitals.
Tell me more about what you mean by rapid response data. How do you set up the kind of system that works?
A challenge for every developing PQC is how to manage data. Figuring out a data system that can help hospital teams drive QI is one of the early key steps in PQC development. From our experience, ideally PQC’s have a system that can provide rapid feedback and that is managed outside of the vital records or state data system. In that scenario participating hospitals feel that the QI data they are collecting is their data for their data reports, and it reduces concerns regarding data being used in more of a regulatory fashion. PQCs use all different sorts of data systems and data sources depending on resources available and on how best to balance data burden for each initiative. Some vital records data, particularly when it can be accessed with rapid turn-around, can be really helpful to PQCs for specific initiatives. From our perspective, having a PQC-managed data system has been helpful in developing hospital team buy-in with participation and data tracking. Providing rapid response data reports provides significant value for hospital teams and certainly helps teams use their data to drive rapid cycle quality improvement.
This goes back to what I was saying about the goal of providing value to the hospital teams. When the hospital teams meet every month, it helps to have simple data reports to review that track progress across time and provide comparisons to other participating hospitals. Ideally they can put the data reports up on the wall and say, ‘This is how we are doing.’ That is real value provided to teams, and it empowers them to make changes within their hospital.
Regardless of the system a PQC is using, we always try to remember that we are not collecting the data for a specific initiative with any reason other than to track the progress of the initiative and give data reports back to the hospitals to drive quality improvement. The best situation is when the hospitals in the collaborative feel ownership of the collaborative and the data system. That makes the teams feel safe being transparent. It also really enables collaboration and sharing between hospitals within the collaborative.
To give that kind of rapid response, do you need someone on staff creating a host of reports every month, or is it automated?
It is automated. That requires a lot of work and thought on the front end, working with a programmer to code a system where hospitals can input key data, through REDCap, and then instantaneously get back the report through a web-based portal.
To achieve that, we decide what reports we want, test them, get feedback, and iterate. That all happens during wave one, where we ask 25-30 hospitals to test the data form and test collecting the data. They give us a lot of feedback on what they think is the best data strategy before they start any QI activity. Is it readable? Is it easy to use? Are we collecting the right data and producing reports that are useful
The data has to be specific to each initiative. You are using the data to drive action for a specific initiative, which means collecting data only for the initiative in front of you, and feeding it back only on that front. If you’re collecting too much data, it ceases to be quality improvement. It becomes a burden, and if hospitals can’t see the benefit they won’t want to participate.
For hypertension, for instance, we tracked four key issues: time to treatment, percent of women who had preeclampsia education at discharge, percent of women who had early follow-up, and percent of cases with a nurse / provider debrief on time to treatment. Just those four things. We tried to make the reports very specific to drive the work.
The data system can be hard for folks, particularly because states have already put a lot of time and resources into systems for collecting vital records, and that typically is a very different system than what seems to be most helpful to support QI. There is a natural tendency to want to make use of the data collection system you already have, rather than invest more time and resources into developing a new system. That is completely understandable, particularly given constraints of budgets and staff resources. But from our experience, our rapid response data system has been really important to our teams and the collaboratives success.
“Collaborative learning” is something that is easy to say, but maybe not so easy to achieve. What does it look like to you, in the context of creating a successful PQC?
In the PQC context we try to be very pragmatic and genuinely collaborative. When we are meeting, whether in person or on calls and webinars, we are focused on what’s in front of us that month, and in the coming months, and on really learning from each other. What are the key strategies this month? How are we doing so far? Can we hear from another state, or from other teams within the state, on what is working and what isn’t? It is very different from having a webinar on how to treat pre-eclampsia, or listening to grand rounds, someone dispensing clinical wisdom. We talk a lot about QI strategies, think about data utilization, work on understanding what the task is in really specific ways and learning from others. It is also really helpful to hear about another team's successful strategies because it makes the challenge feel achievable.
That makes sense when you’re talking about people who are already on board, but how do you drive broader culture and system change? Hospitals are not always eager to change.
Absolutely. If you just put those other things in place, but you don’t convince nurses and providers and hospital administrators why, and how, they need to change their practice, then you are not going to get meaningful changes.
We work on a lot of fronts to support the hospital teams in effecting change within their organizations. The data is a part of that. Rapid response data is great for the teams implementing the initiatives, but it can also be really useful in helping them get buy-in from their hospital. It allows them to demonstrate improvements on the ground as well as the continuing gaps.
The QI support is essential. Some hospitals have a lot of experience implementing QI initiatives, but many don’t. For those hospitals we can help fill in the gaps.
We can also help by providing education and resources to the hospitals. In Illinois we have created a kind of speaker’s bureau, where we have volunteer clinicians who offer to give grand rounds at hospitals. They can come in and say, this is what everyone else is doing. These are the best practices. You should do this too.
We provide toolkits and resources, including some we’ve developed and others from other collaboratives and groups like ACOG and AIM. We’ll print them out and give them to teams. We’ll give them documents they can modify and add their own branding to, make it their own. We provide online training modules for nurses and physicians. Whatever they need to move the ball down the court, whether it is something we have developed, or something another team has done.
Ultimately, though, it can’t rest on us. You need nurse and physician champions to be the charismatic leaders, to convey the urgent sense that implementing this work will lead us to improved care which will lead to better outcomes. You need folks who can step up in the leadership roles and be the people who tell the story, who can conceptualize what we are trying to accomplish.
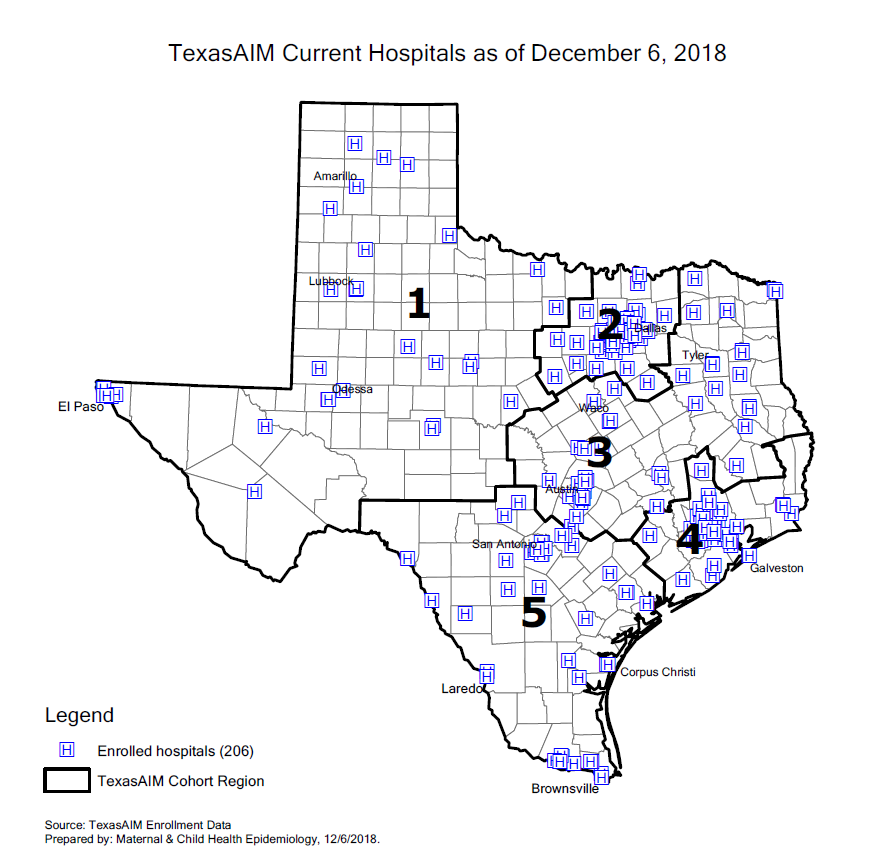
TexasAIM by the Numbers: 206 Hospitals and Counting
As of December 2018, 206 (92%) of Texas’ birthing hospitals are participating in TexasAIM. Of those, 167 are designated “TexasAIM Plus” hospitals, and the other 39 are “TexasAIM Basic” hospitals.
In our last issue, we spoke to Dr. Manda Hall, Associate Commissioner for Community Health Improvement at the Texas Department of State Health Services, about TexasAIM, a new initiative focused on reducing maternal mortality and morbidity in Texas. The initiative, which is being implemented by DSHS in partnership with the Alliance for Innovation on Maternal Health (AIM) and the Texas Hospital Association (THA), will help hospitals and clinics in Texas carry out maternal safety projects.
TexasAIM is launching with an Obstetric Hemorrhage Bundle. The initiative will then focus on the Obstetric Care for Women with Opioid Use Disorder Bundle and Severe Hypertension in Pregnancy Bundle.
As of December 2018, 206 birthing hospitals are participating in TexasAIM. That is 92% of all birthing hospitals in Texas.
As of December 2018, 206 (92%) of Texas’ birthing hospitals are participating in TexasAIM. Of those, 167 are designated “TexasAIM Plus” hospitals, and the other 39 are “TexasAIM Basic” hospitals.
Hospital Enrollment
TexasAIM Basic Hospitals: 39
TexasAIM Plus Hospitals: 167
Total TexasAIM Hospitals: 206
TexasAIM Hospital Cohorts
The AIM Plus hospitals are being divided into five cohorts, by geography, with 20-30 hospitals in each cohort. Each hospital will receive in-person learning sessions from DSHS. They will do an intake assessment, implement the QI bundles, and track and share process and outcome data over time. The hospitals in each cohort are also working together as part of learning collaboratives.
Cohort 1: 32 (16% of enrolled hospitals)
91% of participating hospitals are Plus
76% of hospitals in the region are in AIM
Cohort 2: 47 (23% of enrolled hospitals)
89% of participating hospitals are Plus
98% of hospitals in the region are in AIM
Cohort 3: 40 (20% of enrolled hospitals)
65% of participating hospitals are Plus
95% of hospitals in the region are in AIM
Cohort 4: 44 (21% of enrolled hospitals)
84% of participating hospitals are Plus
96% of hospitals in the region are in AIM
Cohort 5: 42 (20% of enrolled hospitals)
79% of participating hospitals are Plus
91% of hospitals in the region are in AIM
Geographic Area
Rural Hospitals: 74% of Rural Texas Hospitals are enrolled in TexasAIM (17 Basic, 28 Plus)
Urban Hospitals: 98% of Urban Texas Hospitals are enrolled in TexasAIM (21 Basic, 139 Plus)
AIM Data Center Portal
Registered Users in Portal: 402
Hospitals Active in Portal: 191 (93% of enrolled hospitals)
Hospitals with Structure Measures Entered: 176 (86% of enrolled hospitals)
Hospitals with Process Measures Entered: 160 (78% of enrolled hospitals)